It started with routine blood work this spring. I felt fine, but the labs told a different story: my AST and ALT liver enzymes were elevated.
That red flag earned me a referral to a gastroenterologist to discuss next steps. I walked into that appointment expecting a deep dive investigation. What I got was a generic script.
The doctor scanned my blood work values and very quickly, almost nonchalantly, stated: “You most likely have genetically predisposed Fatty Liver.”
He told me he was ordering a liver ultrasound and an elastography, and we would follow up after that. Then, the surreal part happened. Without asking me a single question about what I eat, how I sleep, or if I exercise, he turned away and started dictating notes into his voice recording software while I was still sitting there.
I sat flabbergasted, listening to him tell the computer that I needed to:
- Adhere to a strict Mediterranean diet.
- Exercise for an hour every day.
- Get the scans and check back in 3 months.
That was it. No nuance. No personalization. Just a generic prescription for a complex metabolic problem.
The “Lean Fatty Liver” Paradox
That meeting didn’t provide me with answers, so I did what I always do: I went down the research rabbit hole.
I needed to know what Non-Alcoholic Fatty Liver Disease (NAFLD/MASLD) actually was, how it happened, and if I was stuck with it forever.
The Good News: The liver is the only organ in the body that can fully regenerate itself. This is a reversible disease.
The Bad News: The gold-standard medical advice for reversing it is to “lose 10% of your body weight.”
This is where I hit a wall. At the time of my diagnosis, I had a BMI of around 23.5. While I realized I had a little bit of extra fluff around the waist, I was definitely not obese. Losing 10% of my body weight seemed not only unnecessary but potentially unhealthy if it meant losing muscle mass.
The scary realization hit me hard: You cannot see liver fat in the mirror.

The Self-Audit: How Did I Get Here?
I was already exercising a few times a week. Since the beginning of the year, I had been religiously tracking my food. I wasn’t flying blind, so I dug into my own data to figure out what a lean person does to cause fatty liver.
If I wasn’t overweight, where was the fat coming from?
Looking at my logs, the answer was staring me in the face. It wasn’t “calories” in the abstract sense; it was the source of those calories. My liver fat was likely being driven by processed foods and sugar.
I was definitely the type who “needed” two servings of Double Stuf Oreos after every dinner. I also had a deep love for ice cream (the perfect storm of high saturated fat and high sugar). I was “skinny,” but metabolically, I was flooding my liver with energy it couldn’t process.
The Baseline Data
I believe in tracking progress, not just guessing. Here is exactly where I started.
My Bloodwork (Pre-Intervention):
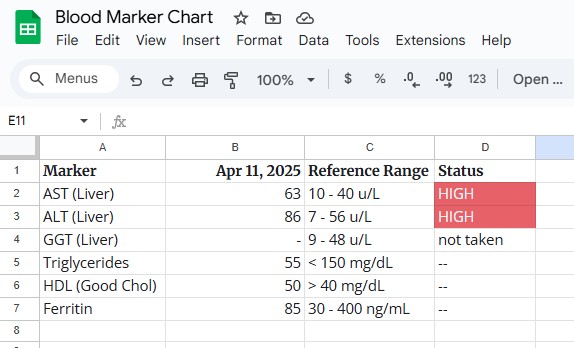
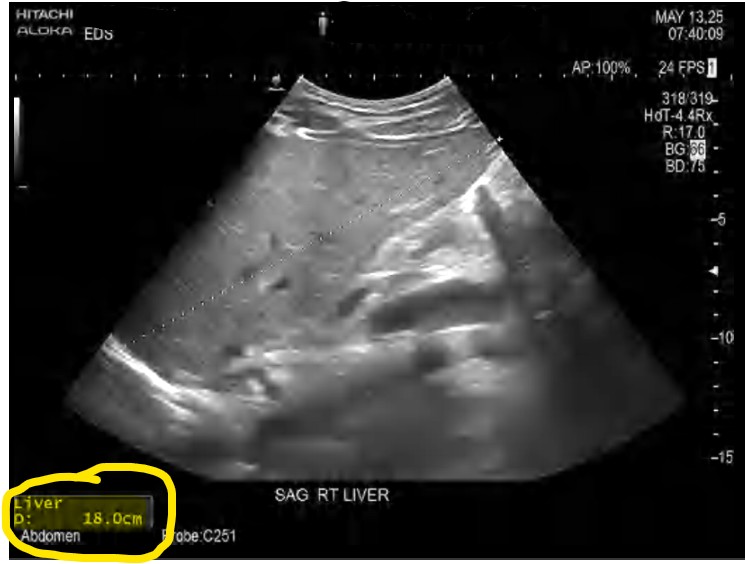
My Ultrasound Results:

Don’t let the word ‘mild’ fool you. In medical terms, ‘mild’ just means I don’t have cirrhosis yet. But looking at the data, my liver was 18c, significantly enlarged. Even though I had a normal BMI and ‘looked fine,’ my liver was inflamed and swollen. This was the wake-up call.
The Path Forward
I am not willing to accept “bad genetics” as an excuse, and I’m not willing to blindly follow generic advice that doesn’t account for my body type.
FattyLiverFighter.com is where I will document my attempt to reverse this condition and keep my enzymes in optimal ranges for good.
I am treating this like a project. My plan involves:
- Diet: A modified, higher-protein version of the Mediterranean diet (to support muscle growth, not just weight loss).
- Fitness: A combination of resistance training and cardio
- Variables: deeply investigating the roles of specific vitamins, stress management, and sleep quality.
I’m not a doctor. I’m just a guy with a spreadsheet and a motivation to fix his metabolic health. If you are in the same boat, especially if you have “Lean Fatty Liver,” I invite you to follow along.
Note: The ultrasound report also noted some echogenicity in my kidneys, which my nephrologist cleared as non-threatening, but it highlights that metabolic stress affects the whole system, not just the liver.
Hey, I also have lean MASLD and have been struggling since I was 14 and 50 kilos. There is a huge lack of support and treatment for us. I myself am a sports player and for my height have great muscle mass but still suffer despite eating zero refined sugars.
Hey Star, thank you so much for sharing your story. It is incredibly frustrating to hear that you’ve been dealing with this since you were 14, but sadly, I’m not surprised by the lack of support. The medical system really struggles when we don’t fit the ‘textbook’ profile of this disease.
It sounds like you are already doing the heavy lifting by avoiding refined sugars and building solid muscle mass through sports. That is huge for protecting your metabolism!
Since you already have the diet and muscle dialed in, have you and your doctor ever looked into the genetic side (like the PNPLA3 gene) or other hidden stressors like sleep/cortisol? Sometimes when the obvious metabolic levers are pulled, it’s those hidden variables keeping the liver inflamed.
Keep fighting. You aren’t alone in this ‘lean’ category, even if it feels like it in the doctor’s office!